A Day of Surgical Simulation at the Chelsea & Westminster
Alex Macdonald
Simon Clarke

Take the incidence of index neonatal surgical conditions, divide by current trainee numbers in the UK, throw in the European Working Time Directive for good measure and then compare the number to an arbitrary indicative one derived from 20 years ago in the “good old days”. Anyone can appreciate that adequate exposure to index operating is a major problem for today’s trainees that isn’t going away anytime soon. One novel solution however, to show competency off the back of an ever-diminishing logbook experience, is surgical simulation.
Simulation as a component of surgical training isn’t anything new and many units offer some form of basic laparoscopy simulation – typically involving punching a few holes in a suitable box and stacking Polo™ mints or other such relatively arbitrary tasks. However, if we are to make a real dent in trainees’ learning curves for neonatal operating and/or meaningfully undertake simulated WBAs (now a recognised option with any PBA) then both a high-fidelity model and a suitably immersive environment are mandatory. That’s why increasingly a number of units and courses are utilising animal models alongside the traditional box with holes.

The Chelsea & Westminster Hospital – the Sloane Ranger’s favourite, is one such unit and has the advantage of a fully-fledged mock up-paediatric operating theatre replete with realistic attributes like a real scrub area, anaesthetic machine and theatre lights that are frustratingly unnecessary complicated to turn on and off. In this environment a truly immersive animal model simulation can be constructed to test both technical and non-technical (team-working) operative skills.
Last week at Chelsea we made use of both the piglet (proud stalwart of many an operative skills course) and the humble chicken. Both procured from a medical meat supplier rather than a civilian butcher who will often remove the important internal clockwork without thinking and hence lessen the experience. Our supplier is the inventively named ‘Medmeat’ ([email protected]) who tick all the appropriate UK/EEC regulatory boxes. The tissue comes frozen and the pig costs ~£90, the chicken ~£10.
Simulated open repair of CDH using blue-coloured patch
With the piglet we simulated an open CDH repair and then a thoracoscopic TOF/OA (which to fix first – the CDH or the TOF/OA? is no doubt a favourite of the veterinary equivalent of the FRCS).
For the diaphragm the piglet makes an excellent anatomically accurate model for the laparotomy approach. A high-fidelity environment is recreated by draping the animal on a (real) operating table and having an assistant and scrub nurse along with a range of real instruments and sutures. If a careful balance is struck with that classic trade-off between adequate defrosting (36 – 48 hours) versus decomposing pig smell, then the tissues feel and behave very similarly to the human infant. Reduction of intestinal contents and the experience of suturing the diaphragm at depth (including patch placement) can be recreated with a high degree of realism.
For thoracoscopic TOF/OA the piglet is an established model that we’ve successfully used on national advanced thoracoscopy courses. It provides a safe and realistic environment in order to practice optimal port placement and the layers of the pig oesophageal wall are particularly well defined making it an excellent model on which to practice taking both mucosa and muscle with each suture.
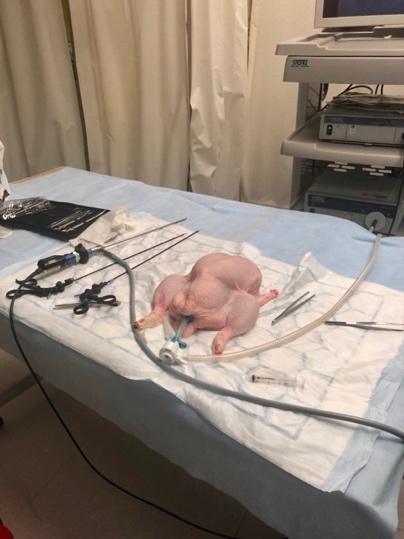
For the chicken, the galliform pneumoperitoneum provides a working space similar to the domain of a neonatal abdomen, but a cursory web search for ‘chicken anatomy’ reveals its shortcomings as an anatomically accurate model. However, it is cheap, compact and we think has potential as a 3mm gallbladder model so we haven’t given up on it yet.
So called ‘wet lab’ simulation – previously the domain of enthusiasts – is moving into the mainstream and can play an increasing role in evidencing competency in paediatric surgical training. Sessions take place every Wednesday afternoon at Chelsea. If you’d like to take part and if you have a particular case you’d like to undertake in a simulated environment then get in touch with Simon Clarke ([email protected], twitter: @sclarke3005).
Alex Macdonald is a Specialist Registrar at Kings College Hospital, Simon Clarke is a Consultant Surgeon at the Chelsea and Westminster Hospital and Chairs the Education Committee at BAPS.
Curated by Mark Davenport