To Ilorin and Back
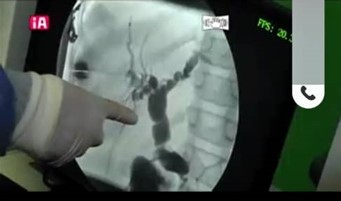 When the call comes through, do you pick up the phone? One day in late March, my colleague in Kings, Niyi Ade-Ajayi, showed me a WhatsApp image of a large choledochal malformation (see left). It belonged to a six-year-old girl who had suddenly become jaundiced in a somewhat unfashionable part of Nigeria – Ilorin (population 1 million). The local paediatric surgeons, were looking for advice on management being a relatively unfamiliar problem over there and not without a risk of post-surgical morbidity and even mortality. Somewhat facetiously I replied – “don’t worry I’ll jump on a plane and we can do the surgery together”.
When the call comes through, do you pick up the phone? One day in late March, my colleague in Kings, Niyi Ade-Ajayi, showed me a WhatsApp image of a large choledochal malformation (see left). It belonged to a six-year-old girl who had suddenly become jaundiced in a somewhat unfashionable part of Nigeria – Ilorin (population 1 million). The local paediatric surgeons, were looking for advice on management being a relatively unfamiliar problem over there and not without a risk of post-surgical morbidity and even mortality. Somewhat facetiously I replied – “don’t worry I’ll jump on a plane and we can do the surgery together”.
They also thought it a good idea to bolster the surgery with some educational content and a 4 day hepatobiliary symposium was born. This was brought together in a matter of weeks with lots of support and contributions from the President of the Association of Paediatric surgeons of Nigeria (APSON) Awwal Abubakar and Emmanuel Ameh, the President of the Global Initiative for Children’s Surgery (GICS) (1) and paediatric surgeon working in the National Children’s Hospital in the capital, Abuja.
There were lots of issues though impeding progress, not the least of which was the administrative thicket that the Nigerian High Commission threw up around granting of the visa. A long wait for a gap in the biometric queue, reams of paper flying down to Ilorin and back confirming the invitation, nature of visit, address of hotel, shoe size, etc. postponed granting of the visa, and a business one at that, to within 24 hours of the flight actually taking off.

Still, having set off as one of the last flights out on a Saturday evening from Heathrow I duly pitched up in Ilorin another flight and 12 hours later to be greeted by the enthusiastic ringmaster of this particular circus – Prof Lukman Abdur Rahman. I had briefly met Lukman in Kings some 15 years previously while he was a BAPS Hugh Greenwood scholar visiting London hospitals. But now, illustrating that BAPS can pick winners, he was head of the department of paediatric surgery in Ilorin.
The surgery was scheduled the following day introduced me to some of the pitfalls of surgery in the tropics. Ilorin is the regional hospital for the state of Kwara and occupies a pretty big footprint in the city, but it is susceptible to some key shortages. So, the ward was completely dark when I met the patient and her mother as the electricity had been turned off, and this remained so for the rest of the week… Its OK Lukman said, they have left it on for the theatres – both lecture and operating. Well, that’s something then.
Live operating video’ed back to a seminar room and thereby transmitted to a Zoom audience of about 100 initially sort of worked, but there was little actual feedback so I have no idea if it was useful. Anyway, we did our little lady with the choledochal malformation and then on the following day repeated it for a baby with possible biliary atresia – it wasn’t and the cholangiogram proved it. Both did well, and discharged a few days later.
The symposium lasted four days, more cases were presented and I did a lot of talking (and listening). Our hepatobiliary service in the UK is free of course, highly centralised and multidisciplinary and any nascent equivalent in this part of the world isn’t. Follow-up is invariably an issue, endoscopy rarely available and it is difficult to find any long-term survivor post-Kasai here so the challenges are huge.

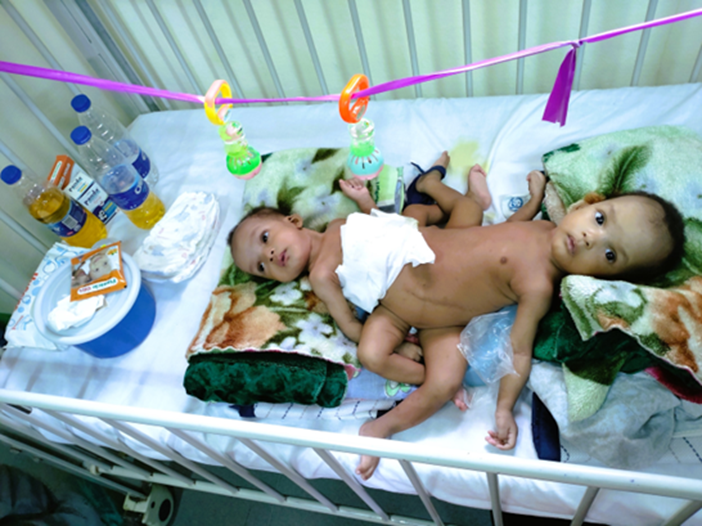
On the way back I had the privilege of a tour around the newest children’s hospital in Abuja (population 3.6 million) which was much more manicured and showed a lot of the basic facilities that Ilorin lacked – all the lights were on for instance– and it even had a helipad for trauma cases. It was also the site of a recently-sited KidsOR (2,3), though locked for the weekend due to staffing issues. I also met surgical cases now rarely seen in the UK such as conjoined twins where the team really has experience, expertise and a great record of success. As to the future? What we both hoped to have created is a sustainable mentored hepatobiliary network – and at least I can say I answered when the call came.
I am grateful to the quick response of the BAPS International Affairs Committee in funding the visa and flights.

Prof Mark Davenport
King’s College Hospital, London
References
- https://www.globalchildrenssurgery.org/
- https://www.kidsor.org/
- Cunningham D, Fedatto M. Building towards equitable access to safe surgery for every child. J Pediatr Surg. 2022 Feb;57(2):182-186. doi: 10.1016/j.jpedsurg.2021.10.026. Epub 2021 Oct 29. PMID: 34857375.